MANAGEMENT OF ACUTE STROKE
- Management Of Acute Stroke
- Case Studies
- Videos
- Testimonials
 Stroke is a medical emergency because brain cells start dying quickly and the treatment is most effective when given promptly. Although some of the cells die within few minutes, surrounding zone though hypoperfused but are receiving just enough oxygen from cerebral blood flow (CBF) to stay alive. A compromised cell can survive for several hours in a low-energy state and is referred to as “penumbra”. If blood flow is restored within this narrow window of opportunity then some of these cells can be salvaged and become functional again. Blood flow to these cells can be achieved by administrating the clot-dissolving thrombolytic agent t-PA by intravenous and intra-arterial routes.
Stroke is a medical emergency because brain cells start dying quickly and the treatment is most effective when given promptly. Although some of the cells die within few minutes, surrounding zone though hypoperfused but are receiving just enough oxygen from cerebral blood flow (CBF) to stay alive. A compromised cell can survive for several hours in a low-energy state and is referred to as “penumbra”. If blood flow is restored within this narrow window of opportunity then some of these cells can be salvaged and become functional again. Blood flow to these cells can be achieved by administrating the clot-dissolving thrombolytic agent t-PA by intravenous and intra-arterial routes.Patients who are able to reach hospital before major infarct has taken place and fulfill the criteria for thrombolysis are the right candidates. Patients with hemorrhage or well-established acute infarct on CT /MRI sequence are not the right candidates. According to the criteria patient’s having hypodensity in less than third of MCA territory on CT scan are eligible for thrombolysis.
Thrombolysis is not done in patients who are likely to have hemorrhage with use of thrombolytic drugs. The contraindications includeCNS lesion with high likelihood of hemorrhage (e.g. vascular malformation, aneurysm, contusion)There are many relative contraindications including mild or rapidly improving deficits, stroke within 3 months, history of intracranial hemorrhage and major surgery within past 14 days. The complete is always checked beore performing the procedure.
n the NINDS trial Favorable outcomes were achieved in 31% to 50% of patients treated with rtPA, as compared with 20% to 38% of patients given placebo. The benefit was similar 1 year after stroke. The major risk of treatment was symptomatic brain hemorrhage, which occurred in 6.4% of patients treated with rtPA and 0.6% of patients given placebo. However, the death rate in the 2 treatment groups was similar at 3 months (17% versus 20%) and 1 year (24% versus 28%).In the NINDS trial there was 11-13% absolute increase in the number of people who had minimal or no disability. When tPA was given within 3 hours of onset of symptoms, the number needed to treat for 1 more patient to have a normal or near normal outcome was 8, and the number needed to treat for 1 more patient to have an improved outcome was 3. These NNT are very impressive.
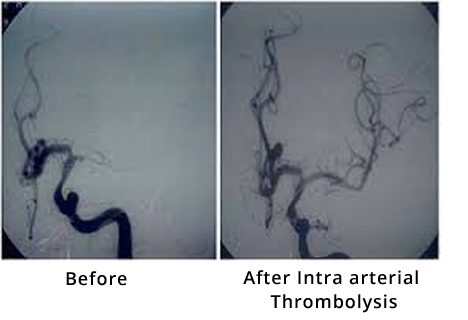 At present intravenous therapy is not recommended beyond 4.5 hours. Intra-arterial thrombolysis can work up to 6-hours. Therefore patients coming between 3 to 6 hours can benefit by intra-arterial therapy. The window period can be further extended in cases of posterior circulation stroke. Patients with major vessel blockage such as internal carotid, middle cerebral artery and basilar artery are unlikely to respond to intravenous thrombolysis and can be treated better by intra-arterial means.
At present intravenous therapy is not recommended beyond 4.5 hours. Intra-arterial thrombolysis can work up to 6-hours. Therefore patients coming between 3 to 6 hours can benefit by intra-arterial therapy. The window period can be further extended in cases of posterior circulation stroke. Patients with major vessel blockage such as internal carotid, middle cerebral artery and basilar artery are unlikely to respond to intravenous thrombolysis and can be treated better by intra-arterial means.Mechanical thrombectomy in acute stroke patient
65 female known diabetic, hypertensive and heart disease presented with sudden onset rt sided weakness with loss of speech since 2 hours. NIHSS 11. MRI Brain with MRA showed acute left MCA infarct with left MCA occlusion. Post mechanical thrombectomy pt made complete recovery.






